Back in the day, autopsy after trauma death was fairly commonplace. Nowadays, it is typically reserved for fatalities that involve a potential crime. And it can be challenging to get the medical examiner to release copies for trauma performance improvement.
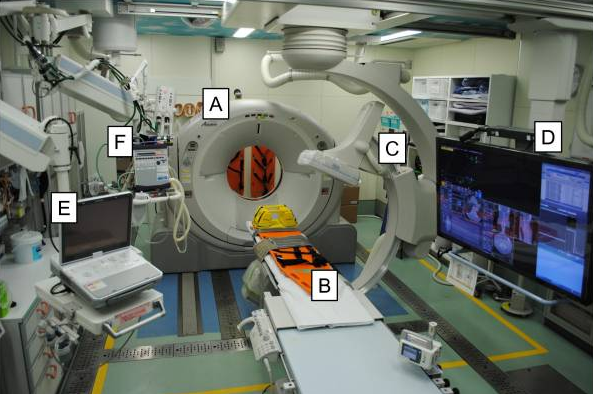
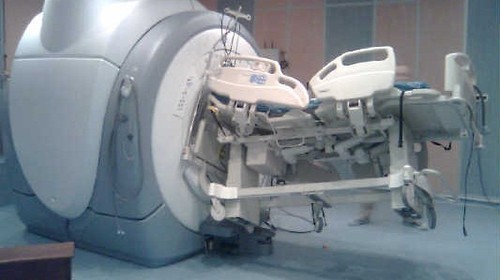
One potential remedy for this began to surface in the literature about twenty years ago: the virtual (or CT) autopsy. This entails sending the postmortem patient to the scanner for head, cervical, chest, and pelvic scans. Although it seems like an exciting idea, there are several logistical issues that I will discuss later.
The trauma group at Indiana University performed a retrospective study to determine the common injury patterns in patients who died at or up to one hour after ED arrival. Their goal was to identify injury patterns that might improve the focus and quality of resuscitative efforts in living patients. They reviewed their experience with doing postmortem CT over a nine-year period. The primary goal was to identify sources of hemorrhage, TBI, and cervical spine injury. They also wanted to identify significant pneumothorax and misplaced airway devices.
Here are the factoids:
- There were 80 decedents in the study, and they were severely injured, with an average ISS of 42
- About three quarters arrested prior to arrival, and the remainder arrived with a pulse
- The most common major injuries were severe TBI (41%), long bone fractures (25%), hemoperitoneum (23%), and cervical spine injury (19%)
- A moderate pneumothorax was present in 19% of cases
- Misplaced airway was identified in 5%
- There was no difference in injury or device mishap patterns between pre-hospital and in-hospital arrest patients (although the number of patients was probably too small to detect one)
The authors concluded that the injury patterns between those who died prior to arrival vs. after were the same. They also noted that patients in arrest should automatically have their chest decompressed and the airway position checked.
Bottom line: This is an intriguing study of a concept I’ve been thinking about for years. The quality improvement benefits could be amazing! Imagine getting immediate feedback on the cause of death and how it might influence future resuscitations. The authors pointed out the power of this with their discovery of missed pneumothorax and malpositioned airways.
But, as mentioned above, there are a host of logistical problems to work out first. Here is a partial list:
- Who accompanies the patient to scan? A nurse? The team?
- Covered or uncovered? It might be creepy for people in the hallways to see a covered person being wheeled around. That’s why hospitals always have those white, wheeled boxes. But it’s equally creepy to see a person who is not moving or breathing being transported.
- Be prepared for your radiologists to gripe about doing free reads
- Where does the report go? It shouldn’t go to the medical record. Or should it?
- What about liability issues? If the team misses something big and the report goes to the chart, it’s fair game for a lawsuit.
- And many more!
Here are my questions and comments for the presenter/authors:
- How did you come to do this study? It appears that your group has been performing CT autopsies for almost a decade. Was there a protocol? Was it done on every eligible patient? If not, could this have skewed your results?
- Do you have the statistical power to detect any differences between the various groups? A few of your results did approach significance. Perhaps more subjects would have helped.
- Tell us how you have addressed the logistical problems above.
This is great work; perhaps it will stimulate a move toward embracing this concept!
Reference: CHARACTERIZATION OF FATAL BLUNT INJURIES USING POST-MORTEM COMPUTED TOMOGRAPHY. EAST 2023 Podium paper #14.