Most trauma centers use an existing venous thromboembolism (VTE) guideline or have developed their own injury-specific one. These include risk factors, contraindications, specific agent, and dosing recommendations. But one thing most do not include is duration of prophylaxis!
The length of time a patient is at risk for VTE is not well delineated yet. The group at the University of Arizona decided to tackle this program using the National Readmission Database. This dataset is a comprehensive resource for critically analyzing patients who are discharged and readmitted, even for multiple occurrences. It covers 30 states and almost two thirds of the population.
The authors focused on VTE occurring during the first six months after injury. Patients who died on the initial admission, were taking anticoagulants, had spinal surgery, or sustained a spinal cord injury were excluded. Over 41,000 records from the year 2017 met these criteria.
Here are the factoids:
- The average age was 61, which shows the skew toward the elderly with these injuries
- Spine areas injured were cervical in 20%, thoracic in 19%, lumbar in 29%, sacrococcygeal in 11%, and multiple levels in 21%.
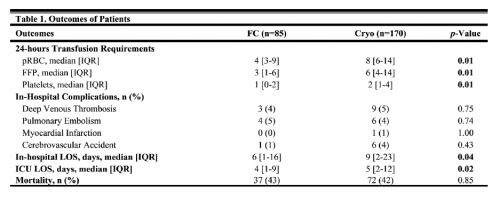
- During the initial admission, 1.5% developed VTE: 0.9% were DVT and 0.7% were PE
- Within 1 month of discharge, 0.6% of patients were readmitted for VTE: 0.4% DVT and 0.3% PE
- In the first 6 months, 1.2% had been readmitted: 0.9% DVT and 0.6% PE
- Mortality in the first 6 months was 6.7%
- Factors associated with readmission for VTE included older age, discharge to a skilled nursing facility, rehab center, or care facility
The authors concluded that VTE risk remains high up to 6 months after conservatively managed spinal fractures. They recommend further study to determine the ideal prophylactic agent and duration.
Bottom line: This is a creative way of examining a difficult problem. We know that VTE risk does not stop when our patient is discharged. This is one of the few ways to get a sense of readmissions, even if it is not to the same hospital. And remember, this is an underestimate because it’s possible for a patient living near a state border to be re-hospitalized in a state not in this database.
This study might prompt us to prescribe up to six months of prophylaxis, particularly in seniors who are discharged to other care facilities.
Here are my questions for the author and presenter:
- Is there any way to extrapolate your data to the entire population of the US, or to compensate for the “readmission over state lines” problem?
- Is the odds ratio of 1.01 for risk of VTE in the elderly age group significant in any way? It seems like a very low number that would be easily overwhelmed by the “noise” in this data set.
- Is the mortality number for all causes, or just VTE?
This is an intriguing study, and one that should influence the VTE guidelines in place at many trauma centers!
Reference: THE LONG-TERM RISKS OF VENOUS THROMBOEMBOLISM AFTER NON-OPERATIVELY MANAGED SPINAL FRACTURE. EAST 35th ASA, oral abstract #28.