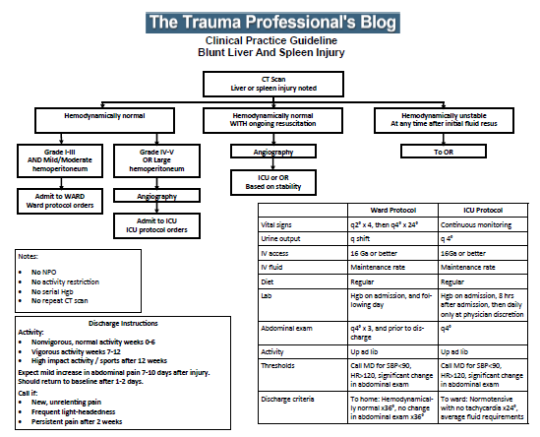
Most trauma centers have some kind of practice guideline for managing solid organ injury. Unfortunately, the specifics at each center are all over the map. Here are a few common questions:
- Should you keep the patient NPO?
- How often should Hgb/Hct be repeated?
- Should they be at bed rest?
- What are their activity restrictions after they go home?
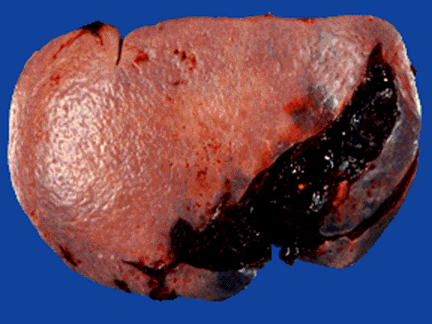
As for activity, some earlier studies have shown that early ambulation is safe. The group at Hahnemann University Hospital in Philadelphia tried to determine if early mobilization would decrease time in ICU and/or the hospital, or increase complications.
Until 2011, their trauma service kept all patients with solid organ injury at bed rest for 3 days(!). They modified this routine to allow ambulation the following morning for Grade 1 and 2 injuries, and after 24 hours for Grade 3 and above, or those with hemoperitoneum. They examined their experience for 4 years prior (PRE) and 4 years after (POST) this change. They excluded patients with penetrating injury, or other significant injuries that would impact the length of stay.
Here are the factoids:
- 300 solid organ injury patients were identified in the PRE period, and all but 89 were excluded
- 251 were identified in the POST period, and all but 99 were excluded
- Hospital length of stay was significantly shorter (5.9 vs 3.7 days) after implementation of the new guideline
- ICU length of stay also decreased significantly, from 4.6 to 1.8 days
- The authors extrapolated a cost savings of about $40K for the ICU stay, and $10K for the ward stay, per patient
- There was one treatment failure in each group
Bottom line: It’s about time we recognized what a waste of time these restrictions are! Unfortunately, the study groups became very small after exclusions, but apparently the statistics were still valid. But still, it continues to become clear that there is no magic in keeping someone starving in their bed for any period of time.
At my hospital, we adopted a practice guideline very similar to this one way back in 2004 (download it below). Hospital lengths of stay dropped to about 1.5 days for low grade injury, and to about 2.5 days for high grade.
And earlier this year, we eliminated the NPO and bed rest restrictions altogether! How many patients actually fail and end up going urgently to the OR? So why starve them all? And normal activity started immediately is no different than activity started a few hours or days later.
Don’t starve or hobble your patients, adults or children!
Related posts:
- Solid organ injury practice guideline (adult) – no NPO or bedrest
- Solid organ injury practice guideline (pediatric) – no NPO or bedrest
Reference: Early mobilization of patients with non-operative liver and spleen injuries is safe and cost effective. AAST 2016, Poster #5.