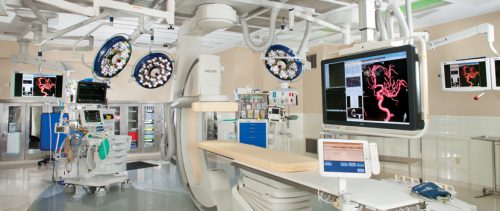
A hybrid operating room is a special suite that allows advanced imaging to be carried out at the same time as one or more additional operative procedures. It’s that simple. It contains specialized imaging equipment including fluoroscopy and infusion equipment for radiographic dye administration. Some also contain CT and/or MRI capabilities, although the shielding required for these makes them very rare. It is generally stocked with a variety of endovascular
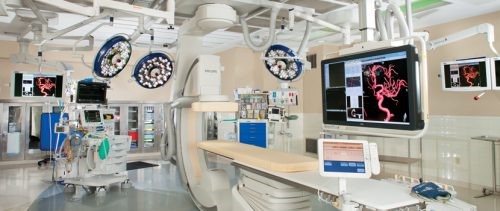
devices and supplies. The usual anesthesia circuits are available, as are selected surgical packs, typically related to vascular and CV surgery.
These suites are typically large, and can easily accommodate multiple operating teams. However, they are very expensive in a number of ways.
First, they take up a great deal of space. Many have the square footage of two or more standard operating rooms. Initial construction costs are very high, as are remodeling and maintenance costs. They can also tax the hospital engineering infrastructure, from electrical to plumbing to ventilation.
But if a hybrid room is available, it can deliver significant benefits to the hospital and to patient care. Intraoperative imaging can provide immediate quality assurance, and patients can undergo more complex procedures and enjoy a shorter length of stay.
Tomorrow, why use a hybrid room for trauma?