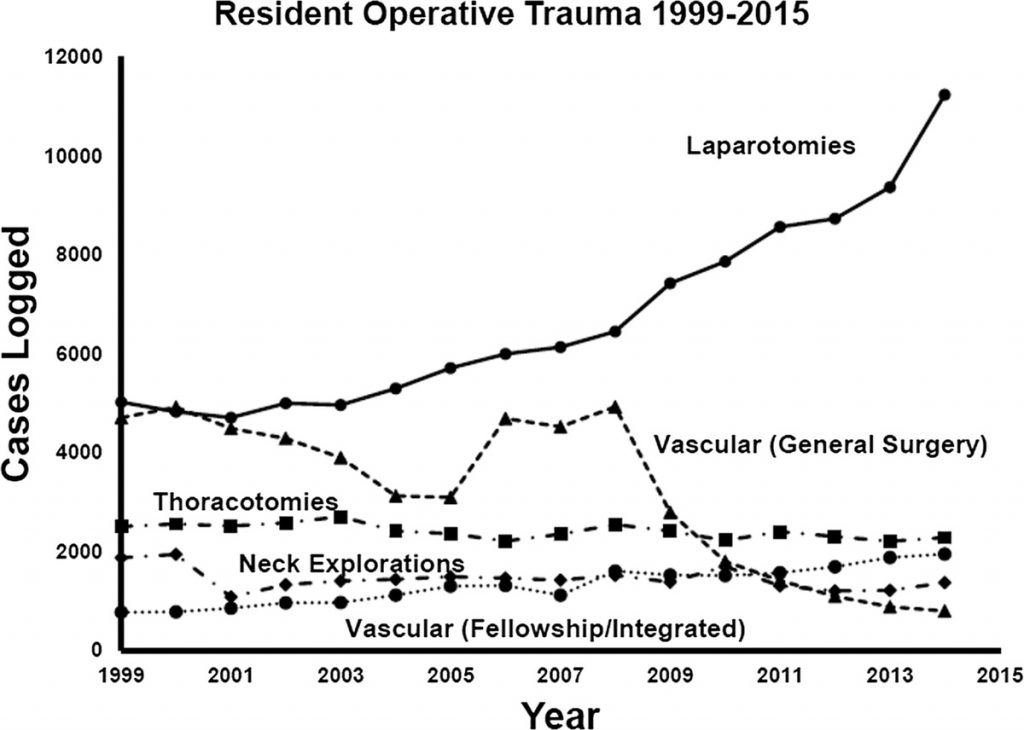
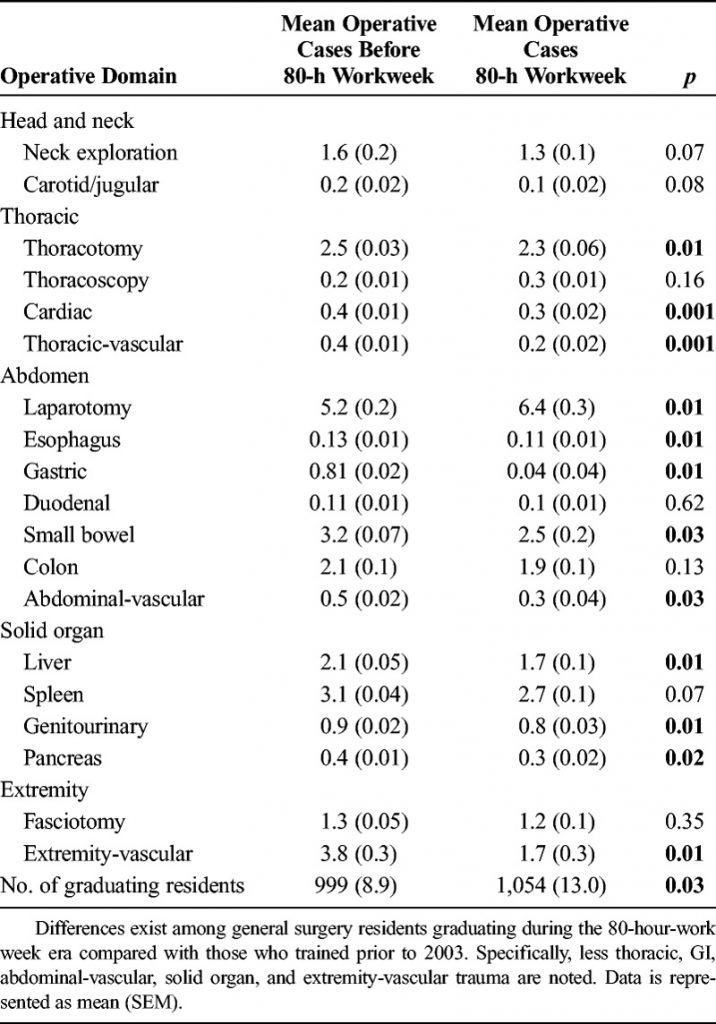
With the implementation of resident work hour restrictions 15 years ago, resident participation in clinical care has declined. In order to make up for this loss of clinical manpower and expertise, many hospitals have added advanced clinical providers (ACPs, nurse practitioners and physician assistants). These ACPs are being given more and more advanced responsibilities, in all clinical settings. This includes performing invasive procedures on critically ill patients.
A study from Carolinas Medical Center in Charlotte NC compared complication rates for invasive procedures performed by ACPs vs residents in a Level I trauma center setting.
A one year retrospective study was carried out. Here are the factoids:
- Residents were either surgery or emergency medicine PGY2s
ACPs and residents underwent an orientation and animal- or simulation-based training in procedures - All procedures were supervised by an attending physician
- Arterial lines, central venous lines, chest tubes, percutaneous endoscopic gastrostomy, tracheostomy, and broncho-alveolar lavage performances were studied
- Residents performed 1020 procedures and had 21 complications (2%)
- ACPs performed 555 procedures and had 11 complications (2%)
- ICU and hospital length of stay, and mortality rates were no different between the groups
Bottom line: Resident and ACP performance of invasive procedures is comparable. As residents become less available for these procedures, ACPs can (and will) be hired to take their place. Although this is great news for hospitals that need manpower to assist their surgeons and emergency physicians, it should be another wakeup call for training programs and educators to show that resident education will continue to degrade.
Reference: Comparison of procedural complications between resident physicians and advanced clinical providers. J Trauma 77(1):143-147, 2014.