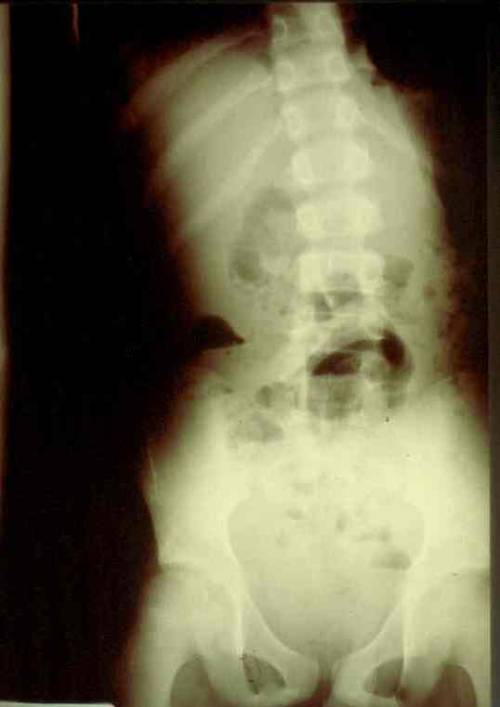
This xray is a classic for a specific trauma surgical injury. Give it your best shot! Tweet of leave comments with your impressions.
This image is especially appropriate for surgical residents / registrars.
Answer in the next post!

This xray is a classic for a specific trauma surgical injury. Give it your best shot! Tweet of leave comments with your impressions.
This image is especially appropriate for surgical residents / registrars.
Answer in the next post!
Blunt injury to the carotids or vertebrals (BCVI) is a little more common than originally thought, affecting about 1% of blunt trauma patients. We have many tools available to help us diagnose the problem: duplex ultrasound, CT angiography (CTA), MR angiography (MRA), and even good old conventional 4 vessel angiography.
But which one is “best?” This is a tough question, because there is always some interplay between clinical accuracy and cost. The surgical group at the Medical College of Wisconsin – Milwaukee did a nice job teasing some answers from existing literature on the topic. The authors tried to take a comprehensive look at costs, including money spent to prevent stroke, the cost of complications of therapy, and the overall cost to society if the patient suffers a stroke.
Here are the factoids:
Bottom line: The “best” test for patients at risk for blunt cerebrovascular injury is the CT angiogram. It minimzes the stroke rate, and provides information on all four vessels supplying the brain, which is probably why the duplex ultrasound has a higher miss rate (can’t see the vertebrals or into the skull). But how do you decide who is at risk for this problem? Tune in to the next post!
Reference: Screening for Blunt Cerebrovascular Injuries is Cost-Effective. J Trauma 70(5):1051-1057, 2011.

This xray is a classic for a specific trauma surgical injury. Give it your best shot! Tweet of leave comments with your impressions.
This image is especially appropriate for surgical residents / registrars.
Answer tomorrow!
Occasionally, patients who have had a severe brain injury but recovered relatively quickly may present with complaints of odd nail discoloration. This may involve fingernails and/or toenails. What gives?

This is actually a byproduct of repeated exams to determine the Glasgow Coma Scale score. A common way to determine the motor component is to squeeze the fingertip or toetip. I’ve seen some neurosurgeons use a pen to apply a great deal of force to the nail.
The discoloration is a resolving subungual hematoma. You may see different colors under different nails, depending on the age of the hematoma. Amaze your colleagues with your knowledge on this one!
When our patients present with a problem, there is a time honored and well-defined sequence to help us come to a final diagnosis.
The first two items are a chip shot, and the trauma professional can gain a lot of information by spending a relatively short period of time doing these. And many times the diagnosis can be made without any further action.
However, diagnostic testing of all kinds has become so prevalent and easy to obtain that we rely on it a bit too much. And sometimes, we order it up in lieu of a thorough history and exam. If the clinician skimps on those steps, it’s much more difficult to narrow the list of differential diagnoses to a manageable number.
So what happens then? They use diagnostic tests as a crutch. Instead of being able to select a few focused tests to answer the questions, they essentially put an order sheet on the wall, fire off a shotgun, and order everything that’s been hit by the pellets.
Lots of tests, so they will definitely find the answer, right? Nope! There are two major problems here. First, the so-called signal to noise ratio is very low. There are so many results, that it is easy to overlook a pertinent positive among all the negatives.
But more significantly, there is always the possibility that there will be more than one positive. One of them might actually be the answer you were seeking. But what about the others? There are the trauma incidentalomas. Some may be truly positive, but there is always the possibility of a false positive. These are the most treacherous, because many trauma professionals then feel obligated to “do something about it.”
As we have found from multiple screening tests like PSA, PAP smear, and mammography, a significant number of patients may be harmed trying to further investigate what turns out to be nothing at all (artifact), or something completely benign. This includes not only harm from complications or unnecessary procedures, but months of anxiety the patient may suffer while the clinicians figure out what that thing inside them really is.
There are only a few studies on trauma incidentalomas available. One reviewed a series of almost 600 head CT scans in patients with TBI and found unexpected findings on 85%. About 90% were obviously benign. Unfortunately, it was not possible to follow these patients to find out how many of the remaining lesions turned out to be benign as well. But I would wager that most did.
Bottom line: I shouldn’t even have to say this, but do a good history and physical exam! If you need diagnostic studies, order only the one(s) that have the potential to make your final diagnosis. Don’t shotgun it. One very helpful tool is a well-designed practice guideline for commonly encountered clinical scenarios. This will limit the number of “other” findings you have to deal with. And finally, did I say to do a good history and physical exam?
Related posts:
Reference: Incidental cranial CT findings in head injury patients in a Nigerian tertiary hospital. J Emerg Trauma Shock 8(2):77-82, 2015.