The debate on how to clear the cervical spine just never ends. We have finally come to some degree of agreement that certain patients (awake, alert, not impaired or head injured, without distracting injury) can undergo clinical clearance alone.
But if those criteria are not met, what next? Universally, adults receive a CT scan of the cervical spine. In the majority of centers, this is coupled with a good clinical examination. And if both are negative, the collar can be removed.
But recent literature suggest that a good, high-quality cervical CT read by a skilled neuroradiologist may be good enough. This has been demonstrated in several papers involving patients who are comatose or other-wise unable to participate with a clinical exam.
Many centers and trauma professionals are still reluctant to remove the cervical collar without that clinical examination. A new study asked the question: would an MRI provide additional, significant information over and above the CT scan in those patients who could not be examined or had persistent neck pain?
A consortium of 8 Level I and II trauma centers in New England participated in this study coordinated by Yale. Blunt trauma patients who underwent MRI after negative cervical CT were considered for the study. On further review, if they received the scan because they could not be clinically evaluated, or if they had complaints of persistent neck pain, they were enrolled. CT scanners with at least 64-slice capabilities were required. There was no mention of the qualifications or special experience of the radiologists reading the images at each center.
Here are the factoids:
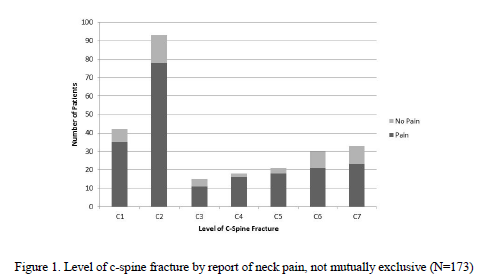
- 767 patients were enrolled in this 30-month study. A total of 43% were for persistent neck pain, 44% for inability to examine, and 9% for both.
- Nearly a quarter had an abnormal MRI scan:
- 17% ligamentous injury
- 4% soft tissue swelling
- 1% disk injury
- 1% dural hematoma
- The collar was removed in most (88%) patients with a normal MRI, but in only 13% with ab-normal MRI
- 11 patients underwent a surgical procedure and half had neurologic signs or symptoms. 10 of them had ligamentous injury, 1 had dural hematoma, and 1 had both
Bottom line: Looks almost compelling, right? One would think that we had better get an MRI on all of these patients! But read more closely, please. Yes, injuries were found. But did they really “require” an intervention? For some injuries, it’s a chip shot. A three column ligamentous injury equals stabilization in any textbook. But management of lesser injuries is less clear. And could some of these injuries have been recognized by a skilled neuroradiologist reading the CT image?
So what to do? There is not enough data for a universal protocol yet. Unfortunately, you will need to develop your own institutional policy based on the experience and opinions of your spine and neurosurgeons. They are the ones who will have to deal with the decision making during and after these studies. Until the definitive study comes along.
Reference: Cervical spine MRI in patients with negative CT: A prospective, multicenter study of the Research Consortium of New England Centers for Trauma (ReCONECT). J Trauma 82(2):263-269, 2017.