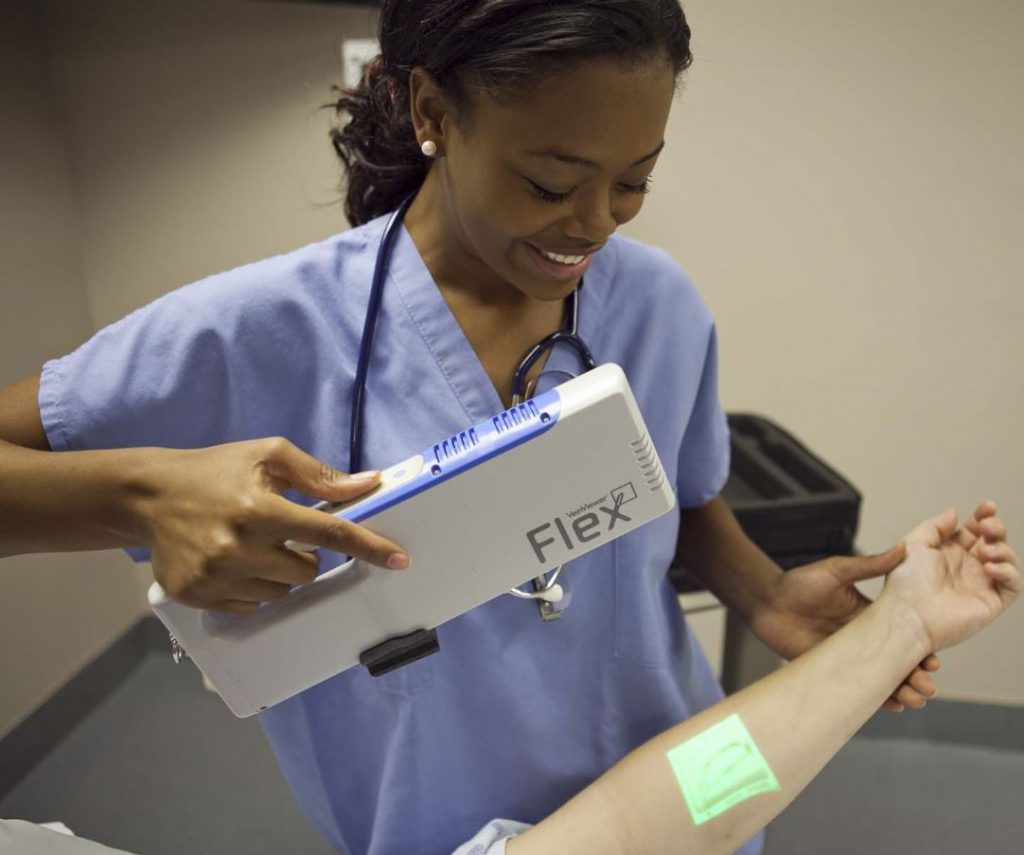
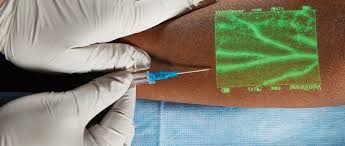
I’m always interested in technology that makes what we do easier, and this item seems to be in the news again. It’s not new technology any more; I first wrote about this way back in 2011. Here’s an objective look at an interesting machine that’s been around for a while. It uses near-infrared light to detect skin temperature changes to allow it to map out veins. It then projects an image of the map in real time onto the skin. In theory, this should make IV starts easier (as long as you can keep your head out of the way of the projector).
One of the first published papers was from Providence, Rhode Island. It evaluated this device to see if it could simplify IV starts in a tertiary pediatric ED. It was a prospective, randomized sample of 323 children from age 0 to 17 looking at time to IV placement, number of attempts, and pain scores.
Unfortunately, the authors did not find any differences. They found that nearly 80% of IVs were started on the first attempt with or without the VeinViewer, which is less than the literature reported 2-3 attempts. This is most likely due to the level of experience of the nurses in this pediatric ED.
The authors did a planned subgroup analysis of the youngest patients (age 0-2) and found a modest decrease in IV start time (46 seconds) and the nurse’s perception of the child’s pain. Interestingly, the parents did not appreciate a difference in pain between the two groups. This may be due to the VeinViewer’s pretty green display acting as distraction therapy for the child.
The Children’s Hospital of Colorado repeated this study and reported their results earlier this year. And unfortunately they had similar findings. There were no significant differences in success rates using the VeinViewer. Also, nurses did not note any difference in their perceived insertion skills or confidence.
Bottom line: Once again, it seemed like a good idea. But that doesn’t necessarily mean that it is. And we always automatically reach for the new shiny toy. This paper points out the importance of carefully reviewing all new (read: expensive at about $20,000 each) technology before blindly implementing it. In this case, an expensive peice of equipment can’t improve upon what an experienced ED or pediatric nurse can already accomplish.
References:
- VeinViewer-assisted intravenous catheter placement in a pediatric emergency department. Acad Emerg Med, 18(9):966-971, 2011.
- Utilization of a biomedical device (VeinViewer® ) to assist with peripheral intravenous catheter (PIV) insertion for pediatric nurses. J Spec Pediatr Nurs. 23(2):e12208, 2018.
I have no financial interest in Christie Digital Systems, distributor of the VeinViewer Vision®.