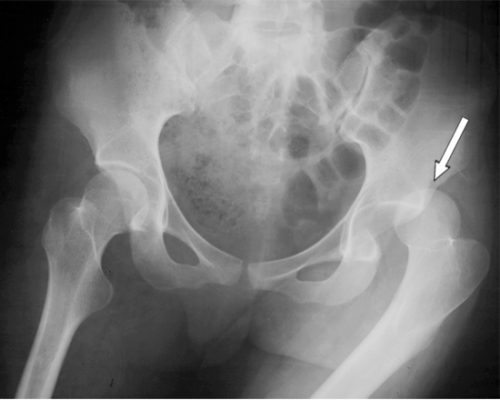
I wrote about posterior hip dislocation and how to reduce it using the “standard” technique quite some time ago (see link below). Emergency physicians and orthopedic surgeons at UCSF-Fresno have published their experience with a reduction technique called the Captain Morgan.

Named after the pose of the trademark pirate for Captain Morgan rum, this technique simplifies the task of pulling the hip back into position. One of the disadvantages of the standard technique is that it takes a fair amount of strength (and patient sedation) to reduce the hip. If the physician is small or the patient is big, the technique may fail.
In the Captain Morgan technique, the patient is left in their usual supine position and the pelvis is fixed to the table using a strap (call your OR to find one). The dislocated hip and the knee are both flexed to 90 degrees. The physician places their foot on the table with their knee behind the patient’s knee. Gentle downward force is placed on the patient’s ankle to keep the knee in flexion, and the physician then pushes down with their own foot, raising their calf. Gentle rotation of the patient’s hip while applying this upward traction behind the patient’s knee usually results in reduction.
Some orthopedic surgeons use a similar technique, but apply downward force on the patient’s ankle, using the leverage across their own knee to develop the reduction force needed. The Captain Morgan technique use the upward lift from their own leg to develop the reduction force. This may be gentler on the patient’s knee.
The authors report a series of 13 reductions, and all but one were successful. The failure occurred due to an intra-articular fragment, and that hip had to be reduced in the operating room.
Reference: The Captain Morgan technique for the reduction of the dislocated hip. Ann Emerg Med 58(6):536-540, 2011.