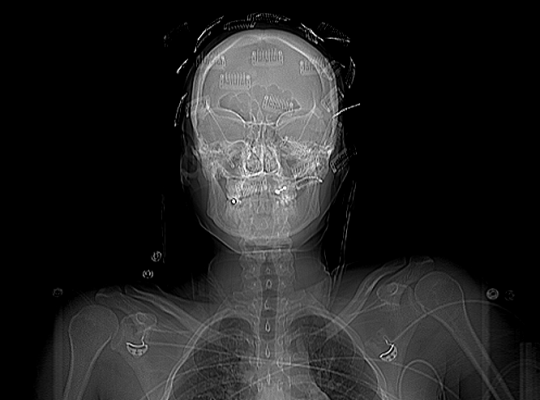
Here’s one for you. A patient is brought to you after a motor vehicle crash. You’ve completed your evaluation in the trauma resuscitation room, and you move off to CT for some imaging.
As the techs are preparing to do the abdominal CT, they perform the scout image to set up the study. This is what you see:
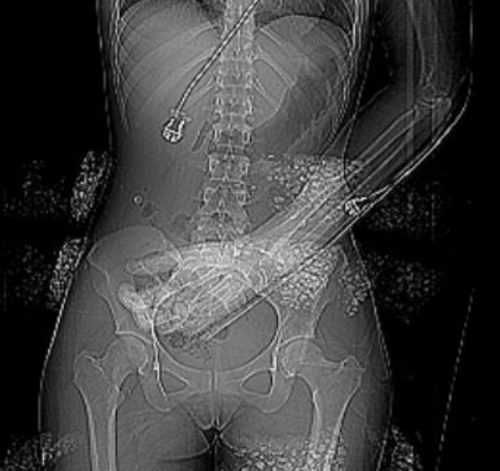
The arm was left down due to a fracture (note the splint along the forearm). But what is all that debris on the image? Other than a few abrasions here and there, nothing is visible on the skin in those areas.
What the heck? What do you think these are? Will they interfere with imaging? And what can you do about it?
Tweet or comment with your answers. I will explain all tomorrow.