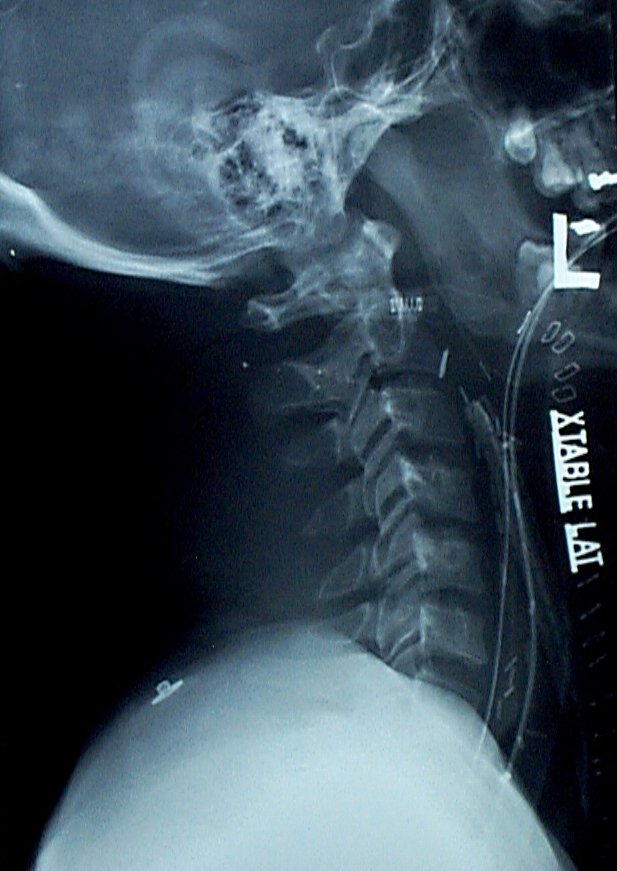
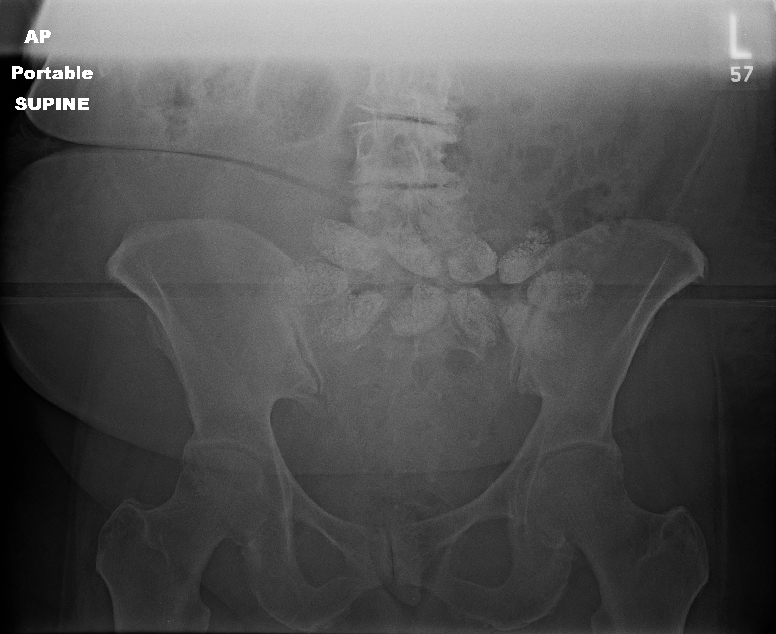
Oftentimes, trauma patients arrive, are not very responsive, and are not carrying an ID. However, our electronic health record systems have a very difficult time with this. To expedite care, most hospitals developed a system of pseudo-names to be used until the patient can be identified.
Originally, these names were often “Doe” names. The classic ones were John Doe and Jane Doe. Obviously, more than two names were needed, so other first names were adopted to provide a sizable pool of pseudo-names. Other disciplines, such as law enforcement, have used a similar system.
Where did the concept of John/Jane Doe come from? The origin is the British legal system, way back in the 18th century. In those days, landlords would start a “process of ejectment,” known these days as eviction, to rid their properties of landlords or deadbeat tenants. The legal process was a bit complex, so they would file for the process using a fake name to initiate it. They frequently selected John Doe or Richard Roe for their filings.
The reason the Doe and Roe names were used has been lost to history. There is speculation that these names were derived from certain deer species endemic to Britain. But honestly, no one knows for sure now. Although this process was dropped in Great Britain in the mid-1800s, it persists in the US legal system. Remember the landmark legal case Roe v Wade?
The use of Doe names in electronic health records is rapidly fading as well. The list of name pairs ending with Doe is just not unique enough. There are too many opportunities to mix up similar names, especially if the last one is always the same. This can result in catastrophic errors if test results are misinterpreted, or a blood transfusion with incorrect ABO typing is given to the wrong patient.
Most trauma centers have adopted temporary naming systems consisting of two words or unique names. Some use number and letter sequences combined with another unique word. The real trick in the electronic medical record world is smoothly merging the records utilizing the pseudo-name with the patient’s previous records under their actual name.
The best practice for this varies by electronic record system and hospital. If done too early, the change may disrupt critical processes, such as the massive transfusion protocol. If done too late, it is difficult for trauma professionals to see any records the patient may have under their actual name. Each center must develop its own system for converting from John Doe to the real name.