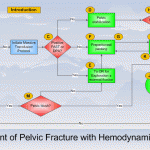
Yes, it is practically dogma that CT should not be used in unstable trauma patients. Either they go directly to the OR, or an attempt to stabilize them is briefly undertaken in the trauma bay. And as you know, I’m not a big believer in dogma. But this one has withstood the test of time. You can see my comments about a previous paper below in the related posts.
But now some authors in Colombia have published a paper that seems to call this idea into question. Could it be true? Read carefully!
This was a small, retrospective review of patients from a large Level I government designated trauma center. They reviewed their experience over a two year period, identifying all hemodynamically unstable patients in the registry. They excluded dead patients, those with isolated head injury, and any who had surgery at an outside hospital prior to transfer.
Here are the factoids:
- 171 patients were reviewed, and of course they tended to be young males
- 91 went straight to the OR, and 80 were taken to CT first
- “Unstable” patients were defined as having SBP < 100 and/or HR > 100
- Mechanism of injury for the OR group was 95% penetrating, but for the CT group was about 50:50 penetrating/blunt
- The mean SBP and HR for the “unstable” patients taken to CT were 92 and 110, respectively
- Mortality was the same for both groups (18% OR vs `13% CT)
Bottom line: The authors concluded that it is permissible to take unstable patients to CT if you don’t spend too much time there based on similar mortality rates. But the problem was that I don’t consider their patients to have been unstable! Mean SBP in their “unstable” group was over 90 torr and the heart rate was only 110! The lowest SBP was only 79. And mortality is too crude of an outcome to rely on. Furthermore, the patients they took to CT tended to have blunt mechanisms, and may not have had ample efforts at resuscitation in the trauma bay first, or may have met criteria to go to CT anyway (see related posts below).
Reference: Computed tomography in hemodynamically unstable severely injured blunt and penetrating trauma patients. J Trauma 80(4):597-603, 2016.