There’s a lot of debate about if and at what age injured children develop significant risk for venous thromboembolism (VTE). In the adult world, it’s a little more clear cut, and nearly every patient gets some type of prophylactic device or drug. Kids, we’re not so certain about at all.
The Children’s Hospital of Wisconsin tried to tease out these factors to develop and implement a practice guideline for pediatric VTE prophylaxis. They prospectively reviewed over 4000 pediatric patients admitted over a 6 year period.
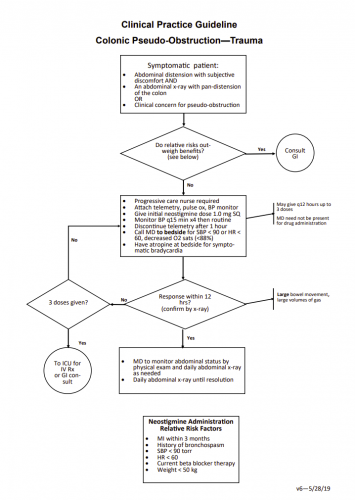
It looks like the guideline was developed using some or all of this data, then tested using regression models to determine which factors were significant. The guideline was then tweaked and a final model was implemented.
Here are the factoids:
- 588 of the patients (14%) were admitted to the ICU, and 199 of these were identified as high-risk by the guidelines
- Median age was 10 (this is always important in these studies)
- VTE occurred in 4% of the ICU patients, and 10% of the high-risk ones
- Significant risk factors included presence of central venous catheter, use of inotropes, immobilization, and GCS < 9
Bottom line: This abstract confuses me. How were the guidelines developed? What were they, exactly? And the results seem to pertain to the ICU patients only. What about the non-ICU kids? The abstract just can’t convey enough information to do the study justice. Hopefully, the oral presentation will explain all.
I prefer a very nice analysis done at the Oregon Health Science University in Portland. I wrote about this study earlier this year. The authors developed a very useful calculator that includes most of the risk factors in this model, and a few more. Input the specific risks, and out comes a nice score. The only issue is, what is the score threshold to begin prophylaxis and monitoring? Much more practical (and understandable) than this abstract. Check it out at the link below.
References:
- Evaluation of guidelines for injured children at high risk for venous thromboembolism: A prospective observational study. J Trauma Acute Care Surg. 2017 May;82(5):836-844.
- A Clinical Tool for the Prediction of Venous Thromboembolism in Pediatric Trauma Patients. JAMA Surg 151(1):50-57, 2016.