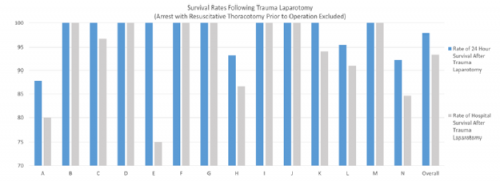
Damage control laparotomy (DCL) has been around now for over 25 years. Many, many papers have been written on its benefits, and the decreased mortality for abdominal trauma specifically. In fact, its use has been generalized to trauma for all other body cavities as well.
However, with this improved mortality came an increase in complications. Incisional hernias remain common, as do episodes of delayed small bowel obstruction. Much of the emphasis in traumatic damage control surgery has now shifted to finding ways to close wounds more quickly and reduce the overall complication rate.
In contrast to damage control laparotomy, much less is known about the potential complications associated with the single-look trauma laparotomy.
This procedure is carried out more frequently than DCL, but we have spent less time studying outcomes and risk factors for complications in this group of patients.
The surgery group at Scripps Mercy Hospital in San Diego conducted a statewide retrospective review of a hospital discharge database of adult trauma patients over an eight-year period. Patients with multiple laparotomies were excluded, as it was assumed that these were damage control patients.
The primary outcomes studied were surgical complications, including bowel obstruction, hernia, fistula, wound infection or dehiscence, and evisceration. Complications were recorded during the initial admission, and during any readmissions in the study period.
Here are the factoids:
- Over 3700 patients were identified as undergoing trauma laparotomy during the study period
- About 2100 were left for review after excluding those with multiple laparotomies (DCL) or an unclear trauma mechanism
- 80% of patients were male and 60% had a penetrating mechanism
- One third of patients were readmitted for a surgery-related complication: SBO 18%, hernia 12%, infection 9%
- Median time to readmission was about 4 months (range 1 week to 1.5 years)
- Patients with blunt injury tended to present with complications earlier (6 days) than penetrating injuries (6 weeks)
Bottom line: This paper is unique in that it is one of the few that was able to follow a large patient population for complications occurring both during and after the initial admission. The overall complication rate was surprisingly high (33%), which is similar to that seen after emergency surgery.
Knowing all of this, what should we do? To date, we have not come close to solving the problems of postop adhesive small bowel obstruction, wound infection, and incisional hernia in any surgical population. However, this work points out the importance of counseling our patients about the potential for complications, how to recognize them, and when to present for evaluation and treatment.
Reference: Outcomes after single-look trauma laparotomy: A large population-based study. J Trauma 86(4):565-572, 2019.