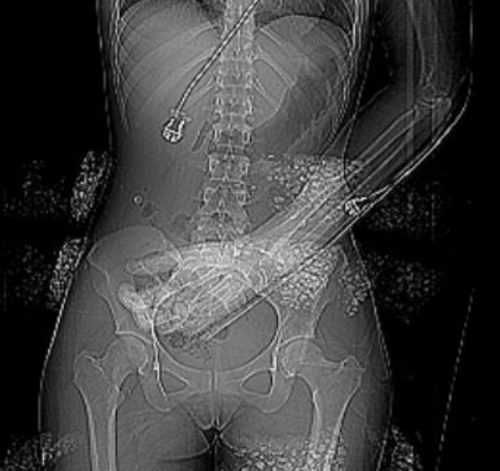
In my last two posts, I described an athlete who developed significant pain in his lower back after rapidly escalating his weight lifting regimen. The pain was very localized to the paraspinal areas bilaterally, and serum CPK was elevated.
Congrats to Jay Slutsky for being the first to figure this one out. The suspected diagnosis was lumbar paraspinous muscle compartment syndrome. Compartment pressures were measured, and were found to be 78 and 26 mm Hg. A contrast MRI was obtained that showed swelling of both sets of paraspinal muscles.
The patient was taken to the OR for fasciotomy.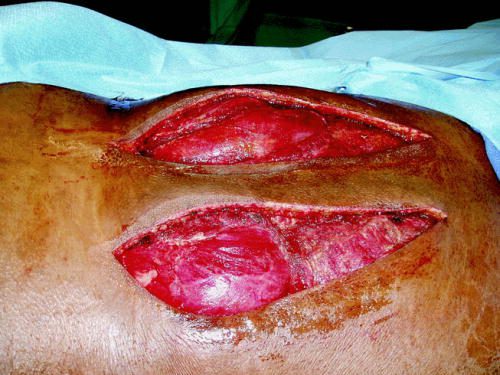 Source: Published paper
Source: Published paper
Note the bulging musculature above. Some areas appeared to be necrotic and did not bleed or contract. There were sharply debrided. The patient recovered quickly, with significant pain relief. The skin incisions were closed after several days, once swelling had subsided. He was well-healed and pain-free at his one month postop visit.
As you can see, any muscle surrounded by a rigid fascial compartment can develop a compartment syndrome. Typically, this requires direct trauma, but exertional compartment syndromes as in this case have been described in the legs of athletes as well. A history of a blow to the muscle group, or of very intense exercise should raise suspicion.
Physical findings of extreme pain that is very focal, coupled with discrete tenderness and firm muscle compartments, should confirm the potential diagnosis. Serum CPK is helpful for trending. Normal pressures in this muscle group tend to be in the single digits to low teens. They rise transiently during exercise, but usually return to normal shortly afterwards. “Normal” compartment pressures are not really known, so findings need to be coupled with CPK levels. Once the compartment pressure reaches the 30s, and especially if accompanied by high and rising CPKs, the syndrome is present. MRI is interesting, but not terribly helpful.
Treatment is typical for any compartment syndrome: release the muscle! A vertical incision centered over the bulging and tight muscle compartment is used. The wound is left open until swelling subsides enough to close the skin. Recovery is usually rapid, although some complain of a persistent low level of pain for a period of time. It is not known how soon these patients may resume sports or training.
Bottom line: Any patient with direct trauma or extreme exertion involving a muscle group is at risk for compartment syndrome. Physical exam, coupled with compartment pressure measurement if in doubt, are the mainstays of diagnosis. CPK levels may help in cases of uncertainty. As with any compartment syndrome, rapid diagnosis and fasciotomy is the key to preserving function and decreasing the likelihood of disability and chronic pain.
Related posts:
References:
- Acute Exertional Lumbar Paraspinal Compartment Syndrome. Spine 35(25):E1529-E1533, 2010.
- Lumbar paraspinal compartment syndrome. International Orthopaedics 36:1221-1227, 2011.
- Paravertebral compartment syndrome after training causing severe back pain in an amateur rugby player: report of a rare case and review of the literature. BMC Musculoskelet Disord 14:259, 2013.