Here’s an interesting case for you to consider. A male victim of an assault is brought to your emergency department with a gunshot to the abdomen. He is met by your team as a trauma activation. Vitals are stable, but he has guarding and rigidity. A single abdominal x-ray is obtained, and then the patient is taken off to surgery. I’ve marked the entry site on the anterior abdominal wall below. There is no exit wound.
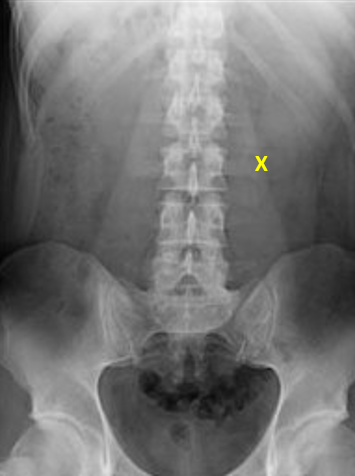
In the operating room a laparotomy is performed. There is a hole in the fascia under the skin penetration. A small hematoma is seen in the underlying transverse mesocolon, well away from the bowel itself. An extensive search is carried out, but no other holes, injuries, or evidence of a bullet is found. Ultimately, the abdomen is closed and the patient is admitted to a ward bed.
WTF? Where did the bullet go? What do you think the possibilities are? Please leave comments today either here or on Twitter. I’ll analyze this puzzling situation tomorrow!
Disclosure for my social media compliance police: this patient was not treated at Regions Hospital, and the x-ray was obtained and modified from the internet.




