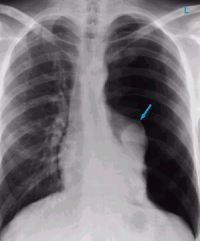
I’ve already written about the (f)utility of serially monitor hemoglobin (Hgb) or hematocrit (Hct) levels when managing solid organ injury nonoperatively. What about if you are concerned with bloody output from a chest tube drainage system? Could it be of any use there?
Seems like a reasonable idea, right? Wrong. As always, think it through and do the math! Here are the questions you need to ask yourself:
- What is the Hgb or Hct of the fluid coming out of the chest tube? At worst, it will be the same as the patient, assuming that pure, whole blood is coming out. But this is seldom the case. The fluid is usually described as “serosanguinous”, which is not very exact, but tells you that it is thinner than blood. And if it looks more like Kool-Aid, the concentration is very low indeed.
- What is the volume in the container? Most collection systems will collect a maximum of 1 to 1.5 L of juice.
- How fast is it coming out? These things almost never fill right in front of your eyes. It’s a slow process, with less than a few hundred ccs per shift.

Here’s a few hundred ccs of thin drainage in a collection system. Probably decrease in Hgb value – < 0.1, which is far less than the range of lab error.
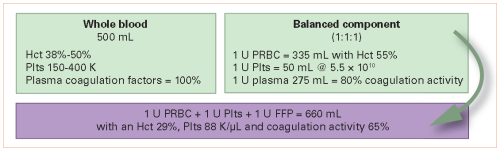
Bottom line: So now do the math. Let’s say the fluid has half the hematocrit / hemoglobin of whole blood. Losing one unit (500cc) of whole blood will generally drop your Hgb by about 1 gm, or your Hct by about 3%. If the blood is half-strength like I am proposing (and the usual drainage is typically much thinner), it will take twice as much (one liter) loss to drop the lab values by that much. This will probably come close to filling up the average collection system. If it takes a day or two or more to fill up, you are not going to see much change in their lab values. And most of the time, the blood in the system is thin like Kool-Aid, so your patient is really losing very little actual blood.
So measuring serial hemoglobin / hematocrit as you watch a hemothorax drain doesn’t make sense. Unless the output is pure blood and the system is filling up in front of your eyes, of course. In that case, a trip to the OR to fix the problem might be a better idea than doing a blood draw and sitting around waiting for the result to come back.
Related post: