The Eastern Association for the Surgery of Trauma (EAST) has published their most recent set of practice management guidelines. This one addresses prevention of falls in the elderly.
All trauma centers and trauma professionals are seeing more and more elderly patients, and the increase in the number of falls among these individuals is alarming. Most trauma centers are already engaging in some kind of prevention activity. However, their falls prevention efforts are all over the map, and there has been little guidance regarding what works and what does not.
So what can be done? The EAST practice management guideline group performed a methodical sweep of the literature to try to give us some objective information to shape prevention efforts. They addressed six specific questions. I have listed them below, with comments on what the literature shows us about the answers.
Question 1: Should bone mineral-enhancing agents be used? Conditional recommendation. A meta-analysis suggests that giving Vitamin D and calcium supplements tends to decrease fall-related injuries. The optimal dosing was not clear, but cholecalciferol doses of 400-800 IU daily and calcium dosing of 1000 to 1500 mg/day were most commonly used. There was a trend toward improved muscle strength and balance.
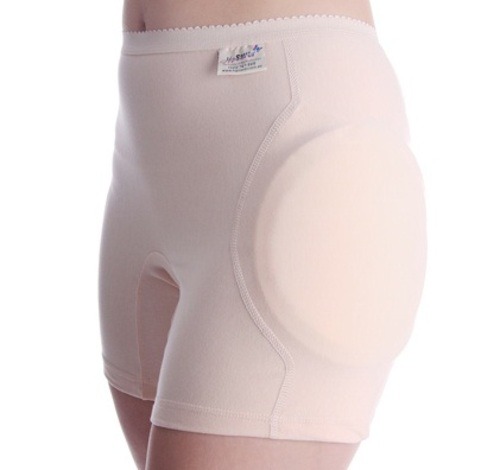
Question 2: Should hip protectors be used? Conditional recommendation.
The evidence does show that wearing protectors decreases fall-related injury. However, compliance is usually an issue because they don’t look very cool. See below:
Question 3: Should exercise programs be used? Conditional recommendation. The literature on exercise routines shows a tremendous amount of variability in terms of the specific routines used. However, most studies do demonstrate a reduction in injury with implementation of an exercise program.
Question 4: Should physical environment modifications be made? Conditional recommendation. Conditions in the household are one of the biggest factors for causing falls. Clutter, throw rugs, poorly placed furniture all increase the risk of injury. The literature is extremely variable in the methods or equipment used, so the results are quite variable as well. Overall, home modifications such as grab bar placement, clutter removal, etc. appear to be of benefit.
Question 5: Should risk factor screening be used? Conditionally recommended. Screening for risk factors is not a specific intervention. However, it can and should be used to identify at-risk patients and direct interventions toward specific risk factors (see next question).
Question 6: Should multiple, tailored interventions be used? Strongly recommended. Research shows that if risk factor screening is applied to individuals or larger populations, and interventions directed at the specific factors identified are implemented, very favorable results are possible.
Bottom line: The best results I have personally seen at other trauma centers have been accomplished through risk factor screening and the use of multiple targeted interventions. Many centers address a single factor, or give talks to groups of older, non-injured patients. Although these activities may make us feel good, they probably don’t have the full effect that multifactorial interventions do, as addressed in Question 6.
Elderly falls are a huge problem (and growing). Every trauma center should work on implementing a comprehensive and multi-factorial falls reduction program. And don’t try to reinvent the wheel. Many centers are already doing this, so don’t be shy about borrowing their program components!
Reference:
Prevention of fall-related injuries in the elderly: An Eastern Association for the Surgery of Trauma practice management guideline. J Trauma 81(1):192-206, 2016.

