You’ve heard the statistics about the graying of our society. The proportion of older people is growing rapidly. Well, there are only about 4400 neurosurgeons in the US, and they are aging as well. Nearly a third are older than 55 years.
This leaves a relatively small number of neurosurgeons tasked with helping to take care of trauma patients. Many Level II centers are hard pressed to maintain their neurotrauma services. Even basic procedures like ICP monitor placement may require transfer to another center.
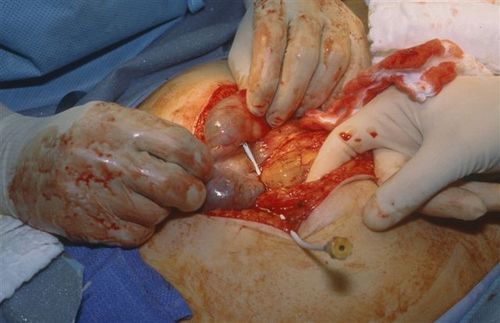
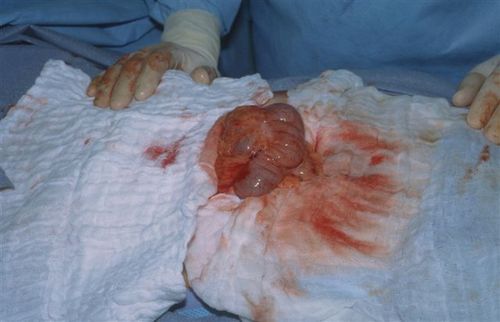
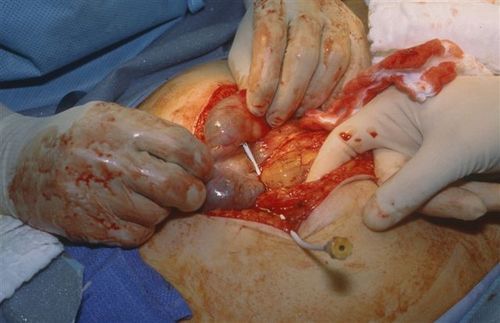
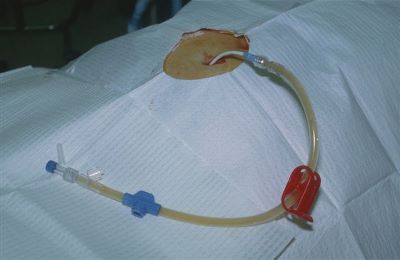
The group at Miami Valley Hospital in Dayton looked at their experience with training surgeons to insert intraparenchymal ICP monitors (not EVD devices) over a 6 year period. Their trauma surgeons, as well as surgical residents were trained by watching a video, practicing in a cadaver lab under the supervision of a neurosurgeon, and being proctored by a neurosurgeon while placing them in three patients. Surgical residents could place the monitor if directly supervised by a surgeon.
Here are the factoids:
- Of 410 monitors placed, 298 were placed by surgeons and 112 by neurosurgeons
- The surgeons placed 188 Licox monitors and 91 Caminos. The type was not recorded in 19.
- Surgeon complication rate was 3% (9 patients), and the neurosurgeon rate was 0.8% (1 patient). None were major of life-threatening.
- Most of the complications were malfunction of the device. There were 2 dislodgements in the surgical group, and 1 in the neurosurgeon group.
Bottom line: This one’s a little tough to interpret. Yes, the number of complications (malfunction) is higher with the surgeons. But the numbers are small, and this difference does not reach statistical significance. I do worry that the training is a bit too sketchy. But I think that this procedure will soon enter the skillset of many acute care surgeons, especially those working at hospitals in more rural settings. This will be the quickest way to begin high quality neurotrauma care for patients who are injured in areas not served by highest level trauma centers.
Related post:
Reference: Successful placement of intracranial pressure monitors by trauma surgeons. J Trauma 76(2): 286-291, 2014.