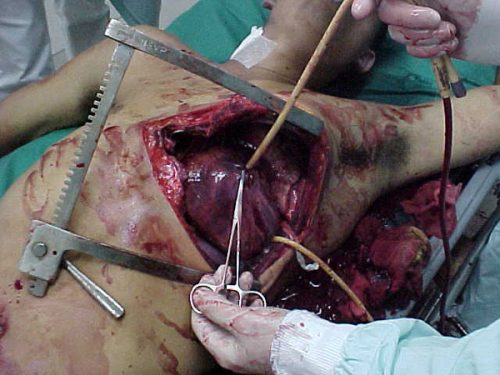
As part of a thorough history and physical on any trauma patient, we typically ask “How big was the knife you were stabbed with?” and “How deep did it go?”
Unfortunately, the answers you typically will get are “This big!” while they hold their hands at least 3 feet apart, and “All the way, doc!”
These answers are not very helpful, so it is not really of much use to ask the questions. The “how big” question is not helpful at all, because a long knife may barely penetrate, and a paring knife can make it all the way into the heart.
This leaves the “how deep” question. There are two ways to determine the answer. If the paramedics or police bring the weapon in, you can carefully examine it (taking proper care to preserve forensic evidence) and see if there is a blood line extending from the tip. This will show the maximum depth of penetration.

The second way is to examine the wound, either by local wound exploration or using CT.
Helpful hint: You can’t tell how large (wide) the blade is by looking at the wound. The elastic nature of the skin causes it to stretch as it is being cut during the stab. When the knife is removed, the resulting laceration will always be less wide than the blade.