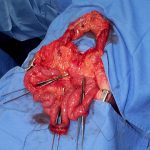
Yesterday, I wrote about the basics of bucket handle injuries of the intestine. Today, I’ll deal with diagnosing them.
An understanding of the mechanism of injury and a good physical exam are paramount. If the patient took a significant blow to the abdomen, especially in a motor vehicle crash (lap belt), be very suspicious. Any abdominal pain is of concern, particularly in the right lower quadrant (most common injury location). If a CT is indicated and there are focal changes in the mesenery or bowel wall, a trip to the OR is advised.
In some patients, the bowel is devascularized and takes 2-3 days to become necrotic. They experience slowly increasing focal pain, and once this develops it’s time to go to the operating room.
Intubated and/or comatose patients can be problematic in making this diagnosis. There is no physical exam, so the trauma professional has to rely on surrogates. The white blood cell (WBC) count is very helpful. The WBC count is typically elevated into the 15,000-20,000 range immediately after trauma, and declines to normal within about 12 hours. If it begins to climb again after 24 hours, especially if it exceeds 20,000, an intestinal injury is likely.
CT scan and abdominal ultrasound are also helpful. A repeat CT scan may show a change in the volume of fluid, or a change in its character. If the amount of fluid increases significantly, or if a fluid bi-layer is seen, a bucket handle injury is very likely. These findings are pertinent in awake patients as well, but the physical exam usually makes use of these diagnostics unnecessary.
Related posts: