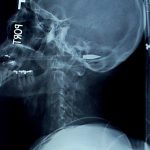
Cervical Spinal Cord Injury: Who Needs A Tracheostomy?
The sad truth is that patients with cervical spine injury may need a tracheostomy. In very high lesions (C1-2) the need may be permanent. Lower injuries (C3-5) frequently need a trach for a limited period of time while they develop enough reserve to compensate for the lost of chest wall muscle power.
It’s not always easy to tell which patient is likely to need intubation upon arrival in the ED. I’ve seen occasional patients fail while getting their CT scans, which is poor planning. Is there a way to predict who might fail, thus benefiting from early intubation and an early plan for tracheostomy?
The trauma group at LAC + USC Medical Center undertook a National Trauma Databank review to try to answer this question. They identified 5256 patients with cervical spinal cord injuries without a severe traumatic brain injury that would otherwise require intubation. About 21% received tracheostomies, and the common predictors were:
- Intubation at the scene by EMS (they’ve done the job of deciding for us!)
- Intubation in the ED
- Complete cord injury at any level
- Facial fractures
- Chest trauma
- Injury Severity Score >=16
Patients who received a tracheostomy generally spent more days on the vent, in the ICU and in the hospital than those who did not. However, their mortality was lower.
It’s generally recognized that patients with complete injuries from C1-C5 routinely require tracheostomy. The surprising thing about this study was that complete injuries at C6 or C7 did as well.
Bottom line: If you have a patient with a spinal cord injury who meets any of the criteria above, stand ready to intubate. I tell my trainees that, if at any time they see something that makes them think about intubating, they should have already done it. Likewise, the surgical ICU team should have a low threshold to performing an early tracheostomy on these patients.
Reference: Incidence of clinical predictors for tracheostomy after cervical spinal cord injury: a National Trauma Databank review. J Trauma 70(1): 111-115, 2011.
Picture: crossbow bolt through the mouth and cervical spinal cord.