It’s one of those time honored treatments that most hospital-based providers are familiar with. The banana bag, reserved for intoxicated patients presenting to the ED or admitted to the hospital. They’ve been around so long, we just take them for granted. But like most things that have become dogmatic, they are due to be questioned from time to time.
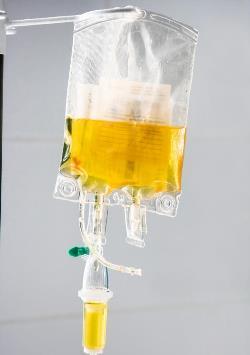
A banana bag is a proprietary mix of “good” stuff, including electrolytes and vitamins, especially thiamine and magnesium. The exact content varies from hospital to hospital. Thiamine and other B vitamins give the resulting solution the characteristic color, hence the term “banana.”
Does it actually do good things like ward off Wernicke’s encephalopathy and megaloblastic anemia? A paper from Jacobi Medical Center in the Bronx prospectively evaluated a series of intoxicated people entering their ED. They drew vitamin B12, folate, and thiamine levels to see if they were deficient enough to even need vitamin supplementation.
Interesting findings:
- These folks (only 77 patients) were very drunk! Average BAC was 280mg/dL.
- Vitamin B12 and folate levels were not critically low in any patient
- Thiamine was low in 15% of patients, but none had clinical evidence of a deficiency
- Later review of prior visits revealed that some patients with low levels had received a previous banana bag within 1 month. Did it do any good?
Bottom line: Most of our intoxicated patients are not vitamin deficient, and don’t need supplementation. The real kicker is that we almost never really try to find out if the patient might be a chronic abuser and potentially at risk. We just hang the bag. Remember, everything we do in medicine has a potential downside. And if the patient really doesn’t need a banana bag in the first place, there is no benefit to balance that risk. The next time you ask for that little yellow bag, think again!
Reference: Vitamin deficiencies in acutely intoxicated patients in the ED. Am J Emerg Med 26(7):729-795, 2008.


