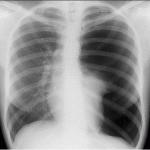
So you’ve been called to the ED to see this 10 year old boy who ran into a buddy on the playground while playing tag. They hit chest to chest, but neither had any apparent injuries at the time. Once home, your patient proceeded to cough up a little blood. Mom promptly brought him to your ED for evaluation.
The first thing to do is a good history and physical. No previous illnesses, nothing like this before. No other obvious injuries, no symptoms of concussion. Just some mild anterior chest wall tenderness in the mid-sternum where he hit the other kid.
Most likely diagnosis: pulmonary contusion. Now, think about what you need to do and the risks and benefits of the tests you could order. What you need to do is rule out a pneumothorax large enough to be treated. A simple chest X-ray will do this. It won’t detect an occult pneumo, but this is not necessary.
A chest X-ray won’t necessarily show you a pulmonary contusion, either. But do you need to see it to make the diagnosis? No! The clinical evidence is enough. A chest CT is almost never indicated in children, and this is certainly not a reason to get one. EKG: not needed unless your pulse exam was abnormal.
if the child has no complaints of dyspnea and appears to be breathing normally, he can go home. This is such a Low energy injury that progression of the contusion is not an issue. Hospitalization offers no benefit, and will certainly inflict more trauma. Instruct the parents to watch for any apparent breathing problems and give typical non-prescription kiddie analgesics if needed. And be sure to tell them that their son may cough up blood for several more days, but it should disappear soon.
Bottom line: unfortunately, we’ve gotten into the habit of ordering lots of tests to confirm things that we already know. We tend to consider the impact in children a little more, especially when it involves radiation. But we really need to start thinking this way for all patients!