Last week I asked for your assistance in determining how big a trauma resuscitation room should be. Thanks to everyone who replied! As you might suspect, these rooms can range from the very spacious…
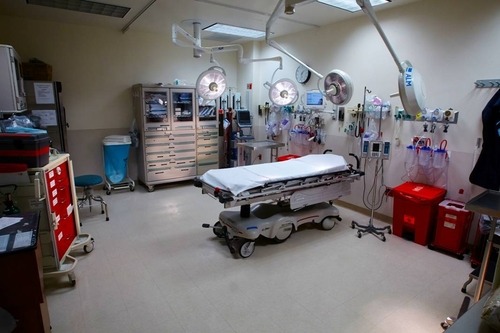
to very tight…
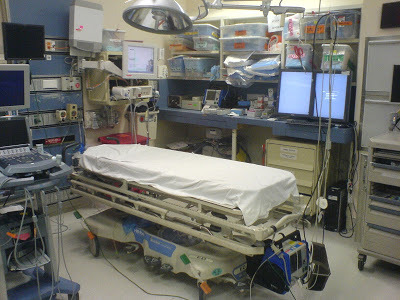
Most respondents indicated that their trauma bays were somewhere between 225 and 300 square feet (21-28 sq meters), although some were quite large (Rashid Hospital in Dubai at nearly 50 sq meters!).
Interestingly, I did manage to find a set of published guidelines on this topic. The Facility Guidelines Institute (FGI) develops detailed recommendations for the design of a variety of healthcare facilities. Here are their guidelines for adult trauma bays:
- Single patient room: The clear floor area should be 250 sq ft (23 sq m), with a minimum clearance of 5 feet on all sides of the patient stretcher.
- Multiple patient room: The clear floor area should be 200 sq ft (18.5 sq m) with curtains separating patient areas. Minimum clearance of 5 feet on all sides of the patient stretcher should be maintained.
The FGI “clear floor area” corresponds to my “Trauma Bay Working Area”, which is the area that excludes all the carts, cabinets, and countertops scattered about the usual trauma room. California’s guideline of 280 sq feet seems pretty reasonable as the “Trauma Bay Total Area”, if you can keep your wasted space down to about 30 sq feet.
Bottom line: Once again, don’t try to figure out everything from scratch. Somebody has probably already done it (designed a trauma bay, developed a practice guideline, etc). But remember, a generic guideline or even one developed for a specific institution may not completely fit your situation. In this case, the FGI guidelines say nothing about the trauma team size, which is a critical factor in space planning. Use the work of others as a springboard to jump start your own efforts at solving the problem.
Related posts:



