After more than 8 years of experience, moving to an electronic trauma flow sheet is still not ready for prime time. I’ve seen many, many hospitals struggling to make it work. And all but a very few have failed.
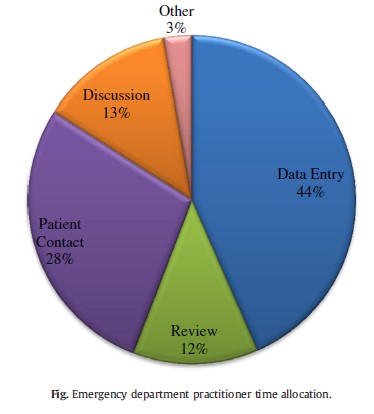
There are two major problems. First, existing computer input technology is underdeveloped. Trying to rapidly put information into small windows on a computer, and having to switch between mouse and keyboard and back is just too slow. And second, output reports are terrible. Humans cannot scan 26 pages of chronological data and reconstruct a trauma activation in their head. There is so much extra data in the typical computer-generated reports, the signal (potential PI issues) gets lost in the noise.
The technology exists to remedy both of the problems. However, the EHR vendors keep tight control over data exchange in and out of their products. Sure, there is CareAnywhere and it’s ilk, but the user is still forced to use the vendor’s flawed input and output systems.
Bottom line: You can’t make a complex system (trauma care) easier or safer by adding complexity (the EHR). Yet.
The electronic trauma flow sheet will never work as well as it could until all the vendors settle on a strong data interchange standard to put data into and get reports out of the EHR. Once that happens, scores of startup companies will start to design easy input systems and report outputs or displays that are actually meaningful. There’s not enough interest in this niche market to make it worthwhile for a company the size of Epic or McKesson, but there is definitely enough for a lot of young companies just chomping at the bit in Silicon Valley.