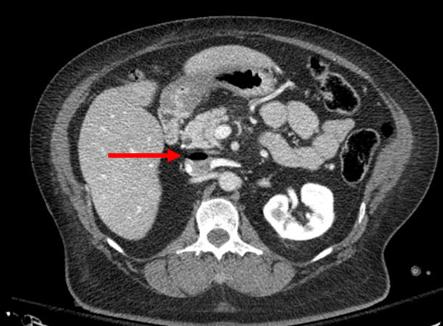
The fifth highest priority taught in the ATLS course is exposure. This generally means getting the patient’s clothes off so any hidden injuries can be identified. Early in my career, I was called to see a patient who had a gunshot to the chest that had been missed because the consulting physician had neglected to cut off her bra. A small caliber wound was found under the elastic strap in her left anterior axillary line after a chest xray showed a bullet in mid-thorax.
The usual trauma activation routine is to cut off the clothes. There are several tips and tricks we use to do this quickly. And a number of commercial products are out there to make it even easier.
But do we really need to cut everyone’s clothes off? I’m not disputing the fact that it’s important to be able to examine every square inch. But do we need to destroy everything our patient is wearing? I once saw a sequined wedding dress cut off (it’s almost as bad as cutting off a down jacket).
The answer is no. The key concept here is patient safety. Can you safely remove the clothing in a less destructive way? For most victims of major blunt trauma, we worry a lot about the spine. Unfortunately, it’s just not possible to allow the patient to wriggle out of their clothes and protect their spine. The same goes for fractures; it may be too uncomfortable to remove clothing because of fracture movement so scissors are required.
Penetrating trauma is a bit different, and in many cases it’s a good idea to try to get the clothing off intact. Once again, if spinal injury is a consideration (gunshots only), the involved clothes should be cut off. A patient with a gunshot to the chest can probably have their pants safely and gently pulled off, but their shirt and coat must be cut.
The police forensic investigators like to have intact clothing, if possible. This is another good reason to try to remove clothing from penetrating injury victims without cutting.
Bottom line: Think before you cut clothes! Major blunt trauma and bad injuries require scissors. Lesser energy blunt injury may allow some pieces of clothing to be removed in the usual method. Most penetrating injury does not require cutting. But if you must (for patient safety), avoid any holes in the fabric so forensics experts can do their job.