Dealing With Shotgun Wounds
Shotgun wounds are uncommon but potentially disabling or deadly. Here are some basics for dealing with them.
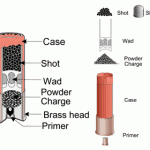
Most people only think about the shot that comes out of the shotgun shell and its effects. While this certainly causes a problem, this foreign body is only a part of it. And it can be challenging to pick them out surgically. However, there are two other foreign bodies that become an issue: the wad, and other material on or around the patient (clothing, pieces of a door, etc).
Look at the diagram above on the left. The wad is a plastic cup that holds the shot and helps the exploding powder charge propel it out of the shell (see sample pictures on the right). If the shotgun is fired at relatively close range, the wad can enter the patient’s wound. It is usually found near the surface and is easily recognized. Be sure to look for it when removing clothing and dressings from your patient.
Any debris from the patient’s surroundings will end up deep to the wad. It is usually centrally located in the wound, and may penetrate as deep as the shot. I once found a piece of coat fabric in the middle of an abscess that formed months after the shooting.
Management of these wounds requires general anesthesia and patience. The soft tissue injury is always worse than it appears, and make take up to 3 days to fully declare itself. I recommend debriding all obviously devitalized tissue and then placing a negative pressure dressing (if possible) to help reduce tissue edema.
All easily found shot should be removed during the initial operation. Deeply embedded particles will either scar in place or migrate to the surface. If all dead tissue is removed, infection is not that common. Inspection of all vital structures, especially blood vessels, should be performed at that time. Remember, due to the velocity and force involved, arteries may appear completely normal on the outside but have significant intimal interruption.
The patient should return to the OR every other day until all tissue die-back has stopped. Final closure or reconstruction can be considered at that time.