Quick and Dirty: Posterior Hip Dislocation
Here’s a quick 5 minute video full of tips on diagnosing and managing this injury. Originally presented at Trauma Education: The Next Generation 2013.
Quick and Dirty: Posterior Hip Dislocation
Here’s a quick 5 minute video full of tips on diagnosing and managing this injury. Originally presented at Trauma Education: The Next Generation 2013.
Today’s big headlines involve the recognition (finally) that law enforcement officers have risky jobs. But not just in the ways you might think. Sure, they frequently deal with criminals who have ill intent or deadly weapons. But some of the risks they face can be mitigated by simple actions.
Here are some factoids:
Unfortunately, a culture has developed among law enforcement (and prehospital / EMS professionals) that seat belts are not necessary (for them). The sad truth is that these professionals are at much higher risk for injury, especially in car crashes, because they must drive faster and in more stressful situations on a regular basis. And police officers (especially in the US) are more and more often confronted with firearms.
Why on earth would they not want this simple protection? Body armor is hot, unwieldy and uncomfortable, especially in warm weather climates. And police officers complain that seat belts complicate getting out of their vehicles, and can get snagged on their utility belts and uniforms.
A number of major police departments and police unions are now pushing for mandatory requirements for seat belts and body armor use at all times. There is now broad recognition that using these devices may cut fatalities in half. Agencies are beginning to check body armor at roll call, and random checks are sometimes performed on the streets by inspectors.
Unfortunately, we need to recognize this problem in EMS as well. And the culture there needs to change, so that protecting the trauma professionals becomes as important as helping the patients that they treat.
Related post:
Reference: Characteristics of Law Enforcement Officers’ Fatalities in Motor Vehicle Crashes. US Dept of Transportation – National Highway Traffic Safety Administration, publication DOT HS 811 411.
Extreme Seat Belt Fail:

This short YouTube video shows a day in the ED at the largest and busiest hospital in the world. The hospital is located in South Africa and is massive, with nearly 3000 beds and covering 173 acres. Over 2,000 patients per day are seen at the hospital, and a large number are trauma victims.
By now, you know the story. Sick little girl who comes to your ED with a rigid abdomen. She’s been previously healthy, and there is no history of trauma.
Here’s the surgical specimen again:
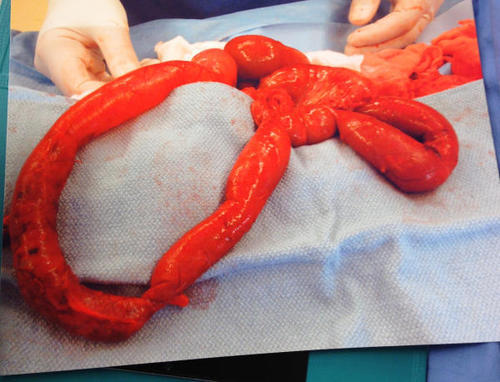
This is a loop of small bowel. It it very inflamed, and you can see a darker color on the portion that is at the left of the picture. This is an area of necrosis, indicating that this portion lost its blood supply some time ago, possibly even a day or two.
A number of readers guessed volvulus or internal hernia, which are on the usual list of differential diagnoses.
But hey, this is the Trauma Professional’s Blog!
Look again carefully at that loop of bowel on the left. There is no mesentery attached to it! This is a classic buckethandle injury. And the only way to get it is from blunt force, typically a car crash. There were also low grade lacerations of the liver and spleen.
What’s the diagnosis now? Non-accidental trauma!
On closer questioning, the father’s story began to change when confronted with this information. As the child recovered from surgery, she underwent a workup and was found to have a number of healed and healing rib fractures of various ages. Child protective services was involved, and the father ultimately admitted to repeatedly striking her in the abdomen in a fit of rage.
Bottom line: Healthy children who are abruptly found to be very ill (or in cardiac arrest) have a high likelihood of non-accidental trauma in addition to the usual medical and surgical culprits. Never lose sight of that, and always maintain some suspicion, no matter how nice the parents seem to be. Treat the child, but always be cognizant of their social/domestic situation!
Yesterday, a child was brought to your ED who looked bad and felt bad, to the point you are convinced she has peritonitis. If the abdominal exam is convincing enough, there is no need for diagnostic imaging It would only serve to add time and radiation to the equation.
If you had really insisted on getting something like a CT, I would have told you that it just showed nonspecific distension and a small amount of free fluid. Helpful, right? And that at the age of 34 she would develop lymphoma for no apparent reason.
Your surgery team takes this patient immediately to the OR and finds this:
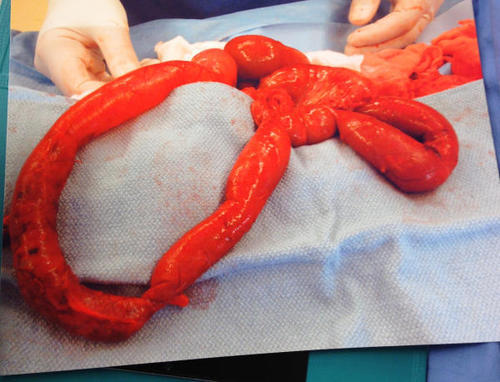
So now my questions are:
Please Tweet and leave emails or comments with your guesses. Discussion and answers tomorrow!