Yesterday, I wrote about proper screening for blunt cerebrovascular injury (BCVI). But, as you know, it’s important to screen only when there is a significant risk of the injury being present. Screening using the shotgun approach (screen everyone for everything) yields enough false positive results to present potential danger to your patient.
A variety of authors on this topic have promoted a number of high risk criteria to trigger a screening test. Most make sense, and are related to the anatomy of the vessels in question. The carotid arteries are relatively unprotected, although a bit deep, as they course up the neck. Thus, it is possible to damage them when they suffer a direct and significantly hard blow. Once they enter the skull, they are better protected. However, fractures through key areas of the skull base and face can injure the vessels, even in these protected locations.
The vertebral arteries are deep and relatively protected as they course through the vertebral foramina. However, if the vertebrae are fractured or subluxed, vessel injury can occur.
Finally, and as always, the physical exam is important. If there are unexpected neurologic changes that can’t be explained by other injuries, or there are indications of deep vascular injury, BCVI needs to be considered.
Here is my list of indications to screen for BCVI:
- Neurologic abnormality not explained by diagnosed injury
- Arterial epistaxis
- Seat belt sign on neck
- GCS < 8 (this is the most commonly forgotten one)
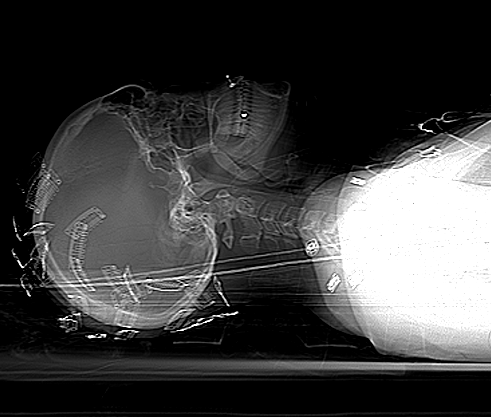
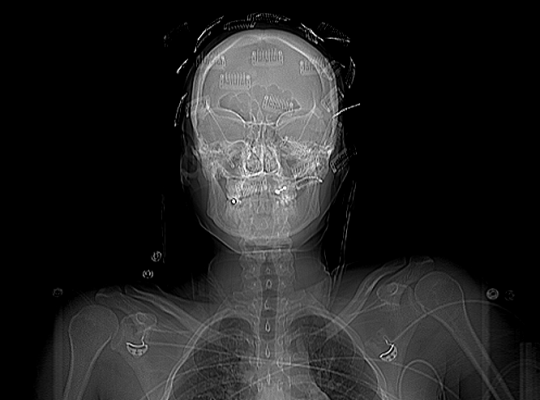
- Petrous bone fracture
- C‐spine fracture (C1‐C3) or subluxation at any level
- Fracture through foramen transversum
- LeFort II or III fractures
Bottom line: Be on the lookout for any of the criteria listed above in your trauma patient. If you find one during your initial evaluation, be sure to order a CT angiogram of the neck. And keep an eye out while scanning the head and cervical spine. If any of the other radiographic indications become apparent, add on the CT angiogram at that point.